Your wellbeing
A healthy workforce is integral to patient safety and to quality and sustainable health care. We support all our members and trainees to make their health and wellbeing a priority.

We’re here to help
As doctors, it can be challenging to balance the demands of a busy profession with family and personal commitments. We too, like the rest of society, can struggle with depression, anxiety and poor mental health.
This page is for wellbeing support in times of personal or workplace difficulty.
Our services and resources
Member Support program (EAP)
RANZCOG recognises that our members can face stressful situations, both in their personal lives and in their demanding yet rewarding professions. This can sometimes result in difficulty maintaining self-care and a healthy work/life balance, which can affect physical and mental health.
To take care of others, you must first take care of yourself. Being proactive about your mental health and wellbeing is important for your professional and personal lives. This involves recognising the signs and seeking informal or professional support when needed.
Our Member Support Program, Converge, provides confidential support to RANZCOG trainees, SIMGs and Fellows (and their immediate family members) across Australia and Aotearoa New Zealand.
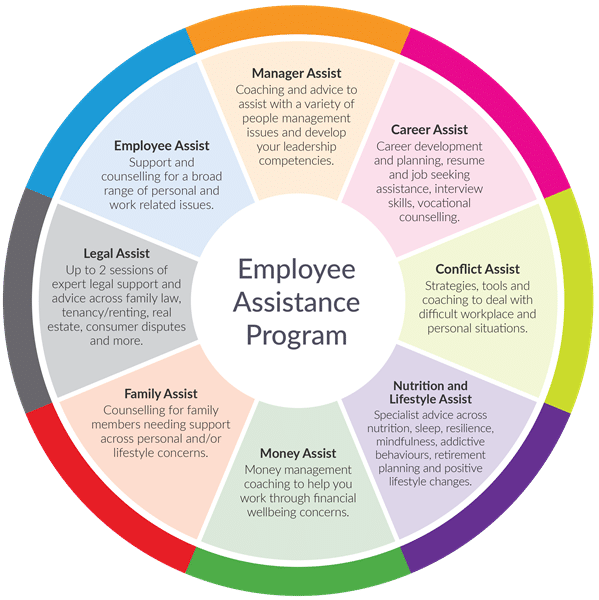
Through Converge, you can access qualified and experienced counsellors on a range of issues including those set out below. Converge also runs specialist helplines for First Nations people, LGBTQIA people and for those impacted by domestic violence. Please ask for these helplines when you contact Converge.
All sessions are entirely confidential, and the College pays for your first four sessions within any 12-month period. Sessions may be face-to-face, by video conference or by phone.
Book a counselling session
Phone
1300 687 327 (Australia)
0800 666 367 (Aotearoa New Zealand)
Online
Further information
Visit the link below to learn more about the process and questions you will be asked when booking your first session.
For any queries, please contact: wellbeing@ranzcog.edu.au.
Trainee and supervisor support
RANZCOG’s Training Support Unit is a confidential service for trainees, SIMGs and supervisors.
RANZCOG recognises that trainees and SIMGs may experience periods of professional and personal difficulty. Coping with the demands of a busy profession, developing skills, building knowledge, as well as balancing family and personal commitments can be challenging.
The College also recognises the importance of supporting supervisors, who ensure trainees and SIMGs receive vital learning opportunities and are given adequate time to develop their skills.
Meet your trainee representatives
Workshops and CPD
To support your mental health and wellbeing, the RANZCOG’s CPD Framework allows for educational health and wellbeing activities to be approved as part of your continuing professional development. If you’re not sure if a wellbeing activity is relevant, please email wellbeing@ranzcog.edu.au.
Wellbeing Advocates
The College Wellbeing Advocates were established in late 2021 and are made up of members and trainees located across O&G departments in Australia and Aotearoa (New Zealand).
The Wellbeing Advocates meet quarterly to share concerns raised in their workplaces and discuss initiatives to better support their colleagues.
Some examples include:
Kindness at Handover (KISBAR): created to better support night shift clinicians during handovers using the ISBAR structured handovers. It involves implementing a designated senior leader as an emotional support person for the team. This person may interrupt any part of the handover that is psychologically unsafe and provides time for one-on-one debriefing for anyone who needs it.
Warm and Fuzzies: created to embed a culture of positive feedback and counter individual tendency for negative self-talk and negative self-reflection (i.e. challenging imposter syndrome). Staff write anonymous compliments to their colleagues which are then read aloud once a week in a teaching setting, called “warm and fuzzies’’.
Wellbeing Advocates can also promote and advocate for proactive mental health and wellbeing support within their workplace; identify, and seek feedback from others, on actions and processes that are causing ill-health; provide feedback to the College on existing initiatives and recommendations for new initiatives; and link trainees and members with relevant College support services and staff representatives.
Health and Occupational Wellbeing Program 2024 (NEW)
Wellbeing Advocates have been invited to pilot the Health and Occupational Wellbeing (HOW) Program within their workplaces in 2024.
The HOW Program is a flexible framework for embedding co-designed wellbeing initiatives in Hospitals and Health Services (HHS). The HOW Program, created by the authors of the Leading with Kindness COVID-19 Toolkit (LKC19TK), aims to leverage the key objectives of the LKC19TK to reduce burnout, improve wellness, and create an ongoing culture of occupational health and safety.
The core purpose of the HOW Program is to empower and guide participants in developing and implementing a tailored wellbeing program for their units to enhance the overall wellness of their team members. The primary output from the project will follow five eLearning modules that will help participants to reflect, plan, and evaluate the impact of implementing the Program. Participants will also be provided with toolkits and templates to support them throughout the process.
Want more information?
If you would like more information on the College Wellbeing Advocates, or are interested in joining, contact wellbeing@ranzcog.edu.au for more information.
You can also join our Wellbeing Advocates Facebook group and follow our Wellbeing Instagram to stay up to date on wellbeing initiatives across the College.
Policies and procedures
Please click on the three dots in the bottom left corner below to explore our policies and procedures relating to member wellbeing.
External services and resources
Health and wellbeing referral options
Australia
Beyondblue: mental health resources and support
Lifeline Australia: support for people in crisis
SANE: support for people with persistent or complex mental health issues or trauma
Perinatal Anxiety and Depression Australia (PANDA): supports people and families affected by anxiety and depression during pregnancy and in the first year of parenthood
Alcohol and Drug Foundation: includes a search tool to find local alcohol and drug services
Aotearoa New Zealand
Alcohol Drug Helpline: information, advice and guidance to help you care for yourself or someone else impacted by alcohol or other drugs.
Lifeline Aotearoa: free and confidential community helplines answered by qualified counsellors and trained volunteers – available 24 hours a day, seven days a week.
Mental Health Foundation of New Zealand: a comprehensive list of helplines and services available in NZ that offer support, information and help.
Tools and digital resources
Leading Kindness COVID-19 Toolkit: a healthcare-specific wellbeing program developed by doctors in training and awarded RANZCOG’s 2021 Group Wellbeing Award.
The Essential Network (TEN): Developed by health professionals for health professionals, TEN provides specialist, individualised mental health advice and triaged support to connect health workers to the help they need.
Smiling Mind: a unique web and app-based program developed by psychologists and educators to help bring balance and mindfulness to people’s lives.
Black Dog Institute: integrating research studies, education programs, digital tools and apps, clinical services, and public resources to discover evidence-based solutions and resources to support better mental health for all Australians. Includes an online clinic.
Shift: an app to safeguard the mental health of JMOs. A free, easy-to-use app designed to help you monitor, improve and maintain your mental health and wellbeing while managing the demands of your profession. Search ‘Shift Black Dog Institute’ on the App Store or Google Play.
RACGP, Keeping the Doctor Alive: a self-care guidebook for medical practitioners (PDF)
MindSpot: free online assessment and treatment for stress, anxiety, depression, trauma and other mental health conditions.
Practitioner advisory services
Australia
DRS4DRS: providing tailored support, online resources and referral services for medical professionals and medical students.
Australian Indigenous Doctors’ Association: supporting Aboriginal and Torres Strait Islander doctors and advocating for a culturally safe healthcare system.
Doctors Health Advisory Service Australia: ensuring every doctor has ready access to health care.
Health Care Worker Wellbeing Centre (Victoria): provides support for people in clinical and non-clinical roles across all health care settings.
Victorian Doctors Health Program: a free, confidential service for Victorian and Tasmanian doctors who have health concerns, including stress, mental illness and substance use.
CRANA: Crana’s Bush Support Services provides free confidential 24/7 telephone psychological support for all rural and remote health workers and their families.
Aotearoa New Zealand
Doctors Health Advisory Service NZ: ensuring every doctor has ready access to health care.
Health and Disability Commissioner NZ: information if a complaint is made about you.
NZ Resident Doctors Association: health and wellbeing information and resources for resident doctors.
Te ORA: Māori Medical Practitioners Associations.
Health and human rights commissions
Medical Association support
Australia
The Australian Medical Association advocates on behalf of the medical profession and the public, operating at a federal level and within each state and territory.
Pacific region
Pasifika Medical Association: a network of health professionals working together to meet the health needs of Pacific people in the region.
Unmoderated peer support groups
Hand-n-Hand
A closed Facebook group that provides a national interdisciplinary peer support network for Australian healthcare workers. Fill out the form here for peer support options including one-on-one support, joining a peer support group or organising a facilitator to provide peer support to your team.
Having your own GP
The Doctors Health Advisory Service has found that fewer than 40 per cent of doctors have an identifiable GP. Many who do are consulting their spouse or practice partner. Many have not consulted that doctor for years.
Find a local health professional
Visit DRS4DRS for information for your annual GP check-up.
Find a local GP, psychologist or psychiatrist who specialises in seeing doctors as patients:
Find a psychiatrist on the RANZCP website: under ‘patient groups’, select the dropdown option, ‘doctors, psychiatrists or medical students’
QLD GPs and psychologists: Doctors’ Health Queensland Find a health professional webpage
SA GPs list: Doctors’ Health SA Find a GP webpage
WA clinical psychologists, psychiatrists and GPs listing: Doctors Health Advisory Service WA Doctors for doctors list
VIC: Contact the Victorian Doctors Health Program for its list of preferred GPs, psychologists and psychiatrists
TAS: Contact the Tasmanian Doctors Health Program (administered by the Victorian Doctors Health Program) for its list of preferred GPs, psychologists and psychiatrists
NT: Doctors Health NT Find a GP webpage
Aotearoa/NZ: DHAS NZ are compiling a list of preferred treatment providers. Please call DHAS NZ on 0800 471 2654 if you’re seeking a treating practitioner.
We can see the value of patients having a personal physician who knows their history and gives personal care, but, in a strange twist of thinking, we don’t see that this applies to ourselves and our families…
So take your own best advice. Find a GP you trust and let them manage your health care. Encourage your colleagues to do the same. This will free you to do what you do best – concentrate on the health of your patients.”
– from ‘Having our own GP‘ by Doctors Health Advisory Service
Adverse outcomes
Medical complications and adverse events happen. The support you receive after an adverse outcome can be crucial to maintaining your wellbeing.
O&G Magazine articles
Facing Adversity, Finding Connection webinar
Hear from senior colleagues about managing adverse outcomes and potential fears going forward if informal channels of support are gone.
For access to a recording of this webinar, please contact: wellbeing@ranzcog.edu.au




Fatigue
Excessive working hours and resulting fatigue can impact both patient safety and doctors’ health.
To support our members, the College has released the Fatigue risk management in obstetric and gynaecological practice (WPI 18) guideline.
Further resources
AMA Fatigue Risk Assessment Tool (online resource)
Mandatory reporting
Seeking help can often instill fear into medical practitioners and raise questions about mandatory reporting.
Advancing system-wide change
RANZCOG has signed up to the ‘Every Doctor, Every Setting’ medical framework, which guides coordinated action on the mental health of doctors and medical students. The College also supports the A Better Culture project, which is working to improve the culture across all health workplaces.
Contact us
Your local office
Local solutions are often the best solutions:
Social media
Join the wellness conversation via our Instagram channel @ranzcogwellbeing

Members
Contact Clare Wells,
Wellbeing and Diversity Lead
Email: wellbeing@ranzcog.edu.au
Phone: +61 3 9412 2977

Trainees and SIMGs
Contact Carly Moorfield,
Training Support Liaison
Email: traineeliaison@ranzcog.edu.au
Phone: +61 8 6102 2096
EAP
We offer short-term counselling and a 24-hour support line through Converge, our Employee Assistance Program (EAP). Enter the organisation code THECMHJ into the online booking form.
